fingernails under microscope
fingernails under microscope-Nails Under The Microscope – Understanding Nail Anatomy & Disorders
Nail technicians should know as much about the inside of the nail as the outside. Here’s an anatomy lesson on the onychium. Pay attention – there’s going to be a test at the end.
While a nail technician’s job is focused primarily on the exterior surfaces of the nail, the supporting structures are just as important, as they dictate how the nails grow. This short lesson will give you the basics of nail anatomy, starting with how the nail is formed in a developing fetus.
The earliest sign of nail development in the embryo occurs at about 10 weeks. On the far end of the finger or toe, there is a pushing in of skin cells, known as an invagination, whereupon a structure called the matrix primordium is found. It is from this source that the true nail matrix develops and begins to manufacture the nail plate, which proceeds to grow outward.
The nail plate, of course, is the external structure. The nail matrix grows underneath the proximal nail fold, which extends back from the cuticle for 1/8 inch to ¼ inch. The matrix ends underneath the nail plate in the lunula – which is not always visible on all nails. Where the lunula ends, the nail bed begins. The nail bed is constructed in longitudinal grooves and ridges and extends distally to where the nail plate just begins to separate from it. This is the site of the hyponychium, which may be seen on an unpolished thumbnail as a very narrow red area that extends from side to side. The hyponychium ends in the normal skin of the finger or toe.
At about 20 weeks, the embryo’s entire nail unit will be fully developed. Underneath the cuticle on top of the nail plate is a very important space called the proximal nail groove. The purpose of the cuticle is to seal off this space and thereby prevent all the outside world hazards from getting in – including bacteria, fungi, and viruses as well as harmful chemicals, soaps, detergents, and so on. That’s why it’s so important no to remove or abuse the cuticle by pushing, cutting, or trimming it.
Sometimes on the nail a thin piece of skin come out from beneath the proximal nail groove and is deposited on the surface of the nail plate. This structure is referred to as the eponychium. It is often confused with the cuticle itself, which is not actually deposited on the nail plate. On both sides of the nail is also a depression into which the nail plate fits snugly. These are known as the laternal nail grooves. They are important as fungus can often enter the nail from those locations.
Finally, the portion of the nail plate beneath the proximal nail fold is called the nail root. It is thinner and softer than the rest of the nail and is easily damaged, particularly by over-manipulation of the cuticle. It is very important to remember that, unlike the skin which has fat underneath it, there is no fatty tissue under the nail. Just beneath the nail unit is bone, called the distal phalanx. The total distance from the surface of the nail plate of the covering (periosteum) of the underlying bone is only about ¼ inch. It is essential to keep in mind that what affects the nail may affect the bone, and what affects the bone may produce an abnormal nail. Consequently, in some cases, an X-ray of the finger or toe can be very helpful in assessing and diagnosing nail disorders.
At the near end of the distal phalanx is a joint known as the distal interphalangeal joint. Old age arthritis (osteoarthritis) can involve this joint, and since it is situated so close to the nail matrix, the nail may be abnormal in clients with this condition. Likewise, the arthritis occurring with psoriasis (psoriasis arthritis) may also affect this joint. The end result is that almost all patients with distal interphalangeal joint psoriatic arthritis have abnormal nails as well.
Fingernails grow at a rate of about 3 mm, or 1/8 inch per month. Toenails grow at about ½ or 1/3 that rate, which is 1-1.5 mm, or 1/16 inch per month. It takes about six months to totally replace a fingernail and 12-18 months to replace a toenail. Nail growth is slower in the elderly, in nails infected by fungus, and during a systemic illness such as a viral infection with fever. Nails grow faster during the summer, pregnancy, menstruation, and in the presence of psoriasis. Frequent trauma or injury may also make the nails grow faster. Because it takes the nails so long to grow, it used to take antifungal medication six months to clear a fingernail and 12 months or more to clear a toenail. With the new treatments available, however, fingernails can be cleared in as few as six weeks, and toenails in only three to four months. This is because the new medications reach the nail very early – one to three weeks – and remain in the nail much longer after the treatment is stopped – three to nine months.
Thus, the anatomy of the nail unit and its adjacent joint and bone structures have a profound effect on nail development and nail disease. Nail growth is also influenced by outside forces that may either speed up or slow down growth according to the particular insult.
Problems with fingernails don’t just happen to adults. Children have nail problems as well, and whether they’re coming to you for services for themselves, or if it’s the child of one of your adult clients, understanding the nail problems of children makes you a more well-rounded nail technician. Nail problems in children and adolescents may often mirror those disorders found in adults. However, there are a number of situations when differences exist.
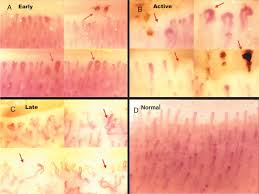
The most common nail condition seen, onychomycosis (fungal nail infection), may occur in young children, although it occurs more frequently in adults. When nail fungus does appear on children’s nails, it is usually associated with a similar infection in one or both parents. The source of the infection, therefore is a parent; many times being related to someone who is prone to onychomycosis (the parent in this case) will leave the child susceptible to onychomycosis, too. Recent data have shown that in a high percent of cases, susceptibility to onychomycosis in inherited. With respect to post-pubertal teenagers, nail fungus can also occur, but overall incidence is also somewhat lower than in adults. The tendency among dermatologists is to treat children with local medications only, such as antifungal creams, gels, solutions, and powders. Because of their side effects, oral medications are generally limited to adults, although in severe or resistant cases they may also be used on children.
Psoriasis of the nails also affects children. The occurrence rate of this disorder is less in children than adults, but if there is a family history of psoriasis, then a particular child may be more susceptible. It is very important for nail technicians to be aware of nail psoriasis, because all too often it is misdiagnosed as a fungal infection. Common signs of this disorder include little dents on the surface of the nail (pits) and separation of the nail plate from the nail bed. In addition, the nail bed may become very thick and have an orange color known as an “oil spot.” The most effective treatment for nail psoriasis is some form of cortisone. In children, we use cortisone creams predominantly, but in adults, cortisone injections around the nails have been very helpful. Physical injury or trauma to the nails may make the psoriasis worse, so remind your clients with nail psoriasis to be extra careful.
Warts around the nails (periungual) and under the nails (subungual) are often seen in children. Unlike nail psoriasis and onychomycosis, peri- and subungual warts occur more often in this age group than in adults. Since viruses cause warts, they can be transmitted from one person to another. It is wise for nail technicians to be aware that that if they are performing procedures using implements on teenagers or children with warts (verrucae) of the nails, not thoroughly disinfecting their implements could spread the disease to other clients. Clients with periungual and subungual warts should be strongly advised to see their dermatologist for medical treatment. Removing warts usually involves some form of surgery, such as burning them off (electrocoagulation) or freezing the off with liquid nitrogen. Your client can use a topically applied wart remover, but they seem to be less effective for treating warts around the nails. Your client can try one before opting for the surgical solution to her wart problem.
Another problem encountered in children are dark bands of the nail extending from the cuticle outward to the nail tip. These bands are usually of more concern in adults than in children. Nonetheless, when seeing such bands, nail technicians should advise the client to seek medical attention. Most of these bands in children are birthmarks. They are like having a mole (nevus) of the matrix, and they may, under some circumstances, require a biopsy or removal. In adults, they are more worrisome because in rare cases they could be a manifestation of a melanoma, a more serious form of skin cancer.
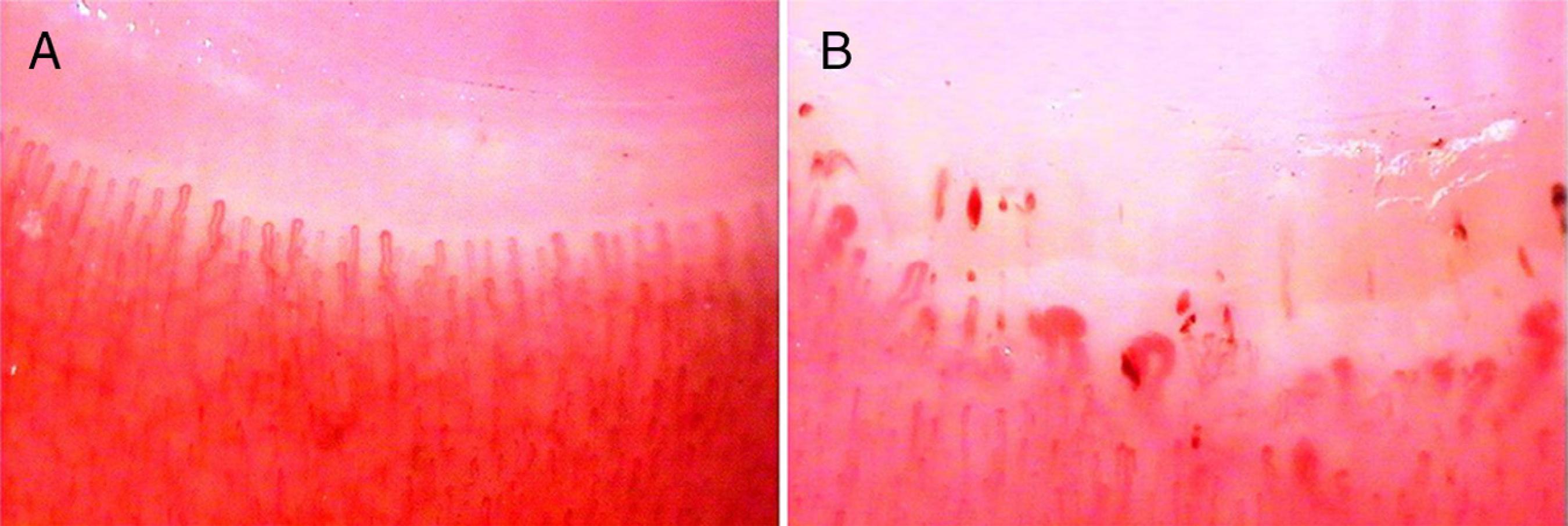
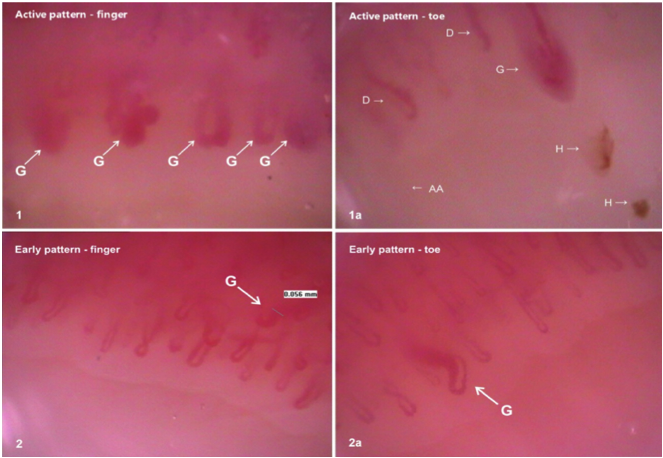
One of the conditions that requires differentiation would be a bruise under the nail (subungual hematoma). Often the patient may not remember an injury that caused the discoloration and thus it is essential for a physician to prove the color is due to blood (from a bruise) and not a possible melanoma. When in doubt, refer the client to her doctor.
A variety of hereditary conditions that affect the nails may signify other more serious health problems, and the nail technician may be in a position to be the first to recognize these conditions and perform a valuable service in recommending medical evaluation.
Some examples include the nail-patella (kneecap) syndrome. With this condition, the nails are abnormal and have triangle-shaped moons. The patient may have no kneecaps and is susceptible to kidney disease.
Another such condition is yellow nail syndrome, where the nails are yellow and have no cuticles. These patients often have swollen ankles as well as lung disease (specifically emphysema, which children do get, but only rarely) and chronic sinus conditions.
A hereditary disorder called dyskeratosis congentia produces very small, thin, and deformed nails and is associated with a seriously low blood count. Again, an astute nail technician will often be the first one to notice some of these abnormalities, and she may be the only one to recognize their significance.
Diabetic children and adolescents are particularly prone to infections around the nails, known as paronychia. With paronychia, the cuticle skin is red, swollen, and somewhat tender. The most common cause is the yeast fungus called candida; nail technicians should not perform any mechanical manipulations around the cuticles, including cutting, trimming, or pushing back the cuticles. Such procedures will make the infection worse and could spread it further, not only in the infected person but to others as well. Again, treatment by a dermatologist is critical; it may include topical and oral medications.
It may be said that the nail technician has a unique opportunity to be a real heroine when young clients come to her salon for services. Although children and adolescent have somewhat different nail problems than adults, they still have much in common. Since the younger age groups are frequenting nail salons more and more often, a heightened awareness among nail technicians can only serve to prove further that they are true professionals with important responsibilities.
Related Items









